Leishmaniasis: Types, Causes, Symptoms, And Treatment
Leishmaniasis occurs mainly in South America, the Middle East, East Africa, Asia, and Southern Europe. An insect from another host or “reservoir” (a disease carrier) spreads leishmaniasis because it is a “vector-borne” infection.
The WHO has a list of “neglected tropical diseases” that includes leishmaniasis. Leishmania pathogens can embody a variety of hosts, including dogs, rats, sloths, cattle, and people.
More than 30 species of sand flies in the Phlebotomus genus can transmit leishmania to humans through bites. Leishmaniasis affects millions of people worldwide, although many Western doctors are ignorant of it. Since the majority of cases may take place in underdeveloped, remote regions without defined reporting systems, it is challenging to estimate the number of cases worldwide.
Leishmaniasis outbreaks of epidemic proportions can happen among people who have been forced into crowded urban areas caused by immigration or war, as well as when high rates of malnutrition weaken residents in affected areas.
Types The majority of Leishmania species are typically found in Dogs and rodents as intermediate hosts. Humans may turn into the main “reservoir” and source of recurrent infection particularly in impoverished, densely populated areas (anthropometric).
There are majorly 3 types of leishmaniasis: visceral (kala-azar) leishmaniasis, cutaneous leishmaniasis, and mucocutaneous leishmaniasis. Leishmaniasis is an infection that affects many different body parts and is caused by a variety of Leishmania species.
To treat leishmaniasis, drugs that are appropriate for the patient’s country of origin, the parasite’s species, and the type of leishmaniasis have been utilized.
Types Of Leishmaniasis
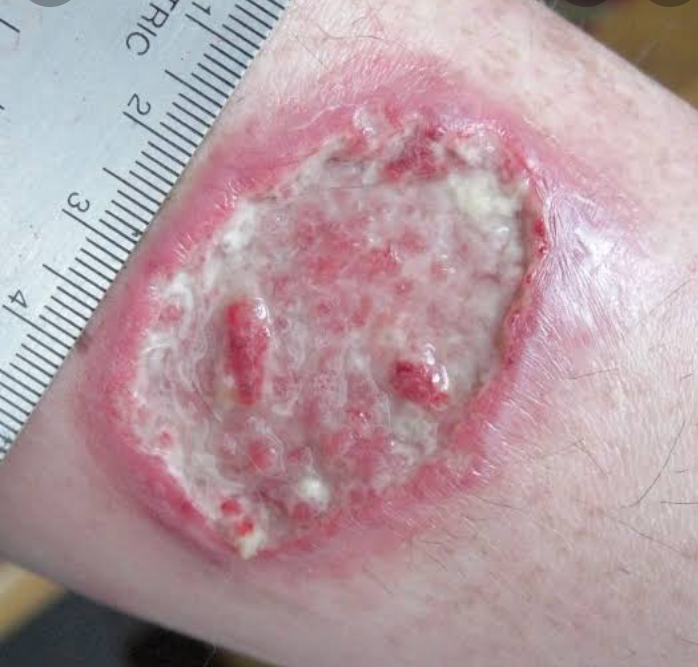
Leishmaniasis is an infection that affects many different body parts and is caused by a variety of Leishmania species. The three syndromes of visceral (kala-azar), cutaneous, and mucocutaneous leishmaniasis are all caused by different species of Leishmania.
Depending on the species of Leishmania, some types can be more prevalent than others in different regions of the world. The symptoms that follow the infecting bite of the leishmaniasis vector could take weeks, months, or perhaps years to manifest.
Sites of Infection of Leishmania
Skin
The skin is the primary site of infection in cutaneous leishmaniasis (CL), the most prevalent type of leishmaniasis. The Middle East, East Africa, Asia (Old World), and Central and South America are where people contract CL the most frequently. Other nations, such as Southern Europe, experience incidences less frequently. Cutaneous leishmaniasis is notably acquired by American soldiers stationed in Afghanistan and Iraq.
In addition to spreading to the tissues of the face and upper respiratory tract, some species of Leishmania also cause CL and, many years later, a mucocutaneous form of the disease. People with weak immune systems may develop disseminated CL, a more severe form of CL with numerous lesions. It might resemble a fungal infection or lepromatous leprosy strikingly.
Mucous Membranes
Mucocutaneous leishmaniasis (ML) is most prevalent in Bolivia, Brazil, and Peru. The nose, nasal septum, mouth, and mid-face are all severely deformed and gradually destroyed by ML. Pneumonia and other secondary infections can be fatal if left untreated.
Visceral Organs
The parasite in visceral leishmaniasis (VL) travels from the skin to the body’s vital organs, namely the liver, spleen, and bone marrow, through the blood and lymph fluids. Compared to CL, this infection type is less frequent but more fatal. In Sudan and India, post-kala-azar dermal leishmaniasis can occur. Months to years after the VL appears to have healed, skin lesions may develop.
In HIV-infected individuals, VL is another significant but underappreciated opportunistic infection. Though cases of HIV-VL have been reported in more than 30 countries, they have primarily been in southern Europe and the Mediterranean, where 70% of people with VL also have HIV co-infection.
Because they lack the cell-mediated immunity necessary for defense and recovery from VL, individuals with immune suppression brought on by HIV are 100–2,000 times more likely to experience severe VL.
As a result of the parasites’ rapid growth, these people also develop into potent human reservoirs, frequently spreading both HIV and Leishmania through the use of Intravenous drugs. When populations with HIV and a co-infection migrate, it is alarming that VL may follow.
Causes Of Leishmaniasis

Parasitic Protozoa
Leishmaniasis is brought on by parasitic intracellular protozoa from the genus Leishmania. Small in size, the organisms. Leishmania affects people from over 20 different species.
When an infected sand fly bites you, you develop leishmaniasis. Inside the sand fly female, the parasite thrives and multiplies. The warmer months, from dusk to dawn, are when this insect is most active, preferring humid environments.
Infected Pets
Dogs, among other domesticated animals, can act as the parasite’s reservoir. Animals, sand flies, and humans could all transmit disease.
Blood Transfusion
A blood transfusion or the use of contaminated needles can also spread the parasite between people. The parasite enters the amastigote stage and starts multiplying after entering the human mononuclear cells. It then spreads to other cells and tissues. Transmission from a human to sand fly to a human is also possible in some regions of the world.
Feotal Transmission
Leishmania can spread from the mother to the fetus during pregnancy.
Symptoms And Signs Of Leishmaniasis
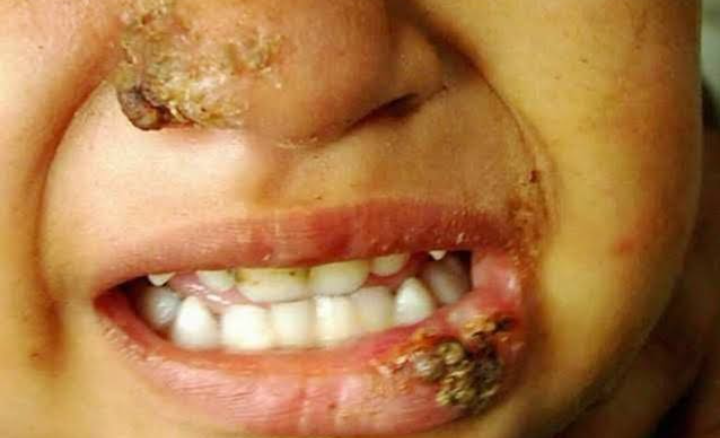
According to the type of leishmaniasis present, leishmaniasis symptoms and signs typically vary.
Visceral leishmaniasis, also known as kala-azar, can range from mild to severe. Some patients are asymptomatic and are unaware that they are parasite carriers.
After the sand fly bite, symptoms can take weeks or even months to manifest. Less frequently, when someone’s immune system is suppressed, symptoms don’t show up for years. These are the five traditional signs of a more serious illness:
Possibly drastic weight loss, low blood levels (pancytopenia), liver and spleen enlargement (hepatosplenomegaly), which may cause the abdomen to swell, fever, which is usually intermittent, and high levels of immune globulin in the blood (hypergammaglobulinemia).
VL is known as “kala-azar,” which translates to “black fever” in Hindi, due to the possibility of hyper-pigmentation in very advanced diseases in India. Increased melanin in the skin is what causes hyperpigmentation.
The pituitary gland is stimulated to produce high levels of the adrenocorticotropic hormone as a result of the inflammatory products caused by VL, which increases the production of melanin.
When VL is effectively treated, hyper-pigmentation typically disappears. Because of earlier treatment, it no longer occurs as frequently. Although some anti-leishmanial medications might also be to take some responsibility for kidney toxicity, thus it tends to affect the kidney, which could result in renal failure. Other organs, such as the bowel and the lung, may also be impacted by leishmaniasis.
Other names for dermal or cutaneous leishmaniasis (CL) include “pian bois” and “chiclero ulcer” in South America, “Aleppo boil” in the Middle East, and “Delhi boil” in India, among many others.
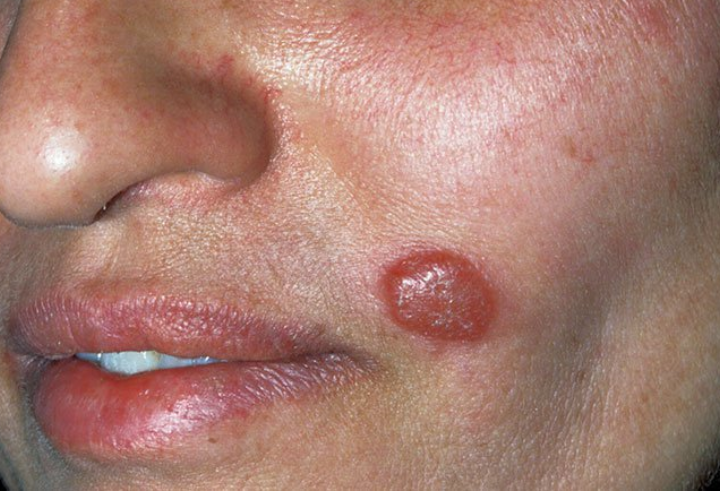
Typically, the bite site of a sand fly develops a raised papule with a piled-up border that enlarges and ulcerates. It takes the illness several weeks to show symptoms. A single lesion might exist, or over time, more might develop.
The skin lesions can resemble psoriasis, warts, acne, or other conditions depending on their appearance. Large, scaly, ulcerated plaques or shallow ulcerated nodules may be how they present themselves.
The extremities and face are the most common places for sores to appear. Nodular lesions may be widespread and last for years or even the rest of one’s life in severe cases, such as diffuse cutaneous leishmaniasis.
The nose, mouth, and larynx are all affected by mucocutaneous leishmaniasis (ML). Compared to VL and CL, it is less typical. At first, the patient develops a nodule at the site of the sand fly bite along with symptoms of CL.
Mucocutaneous involvement subsequently causes nasal nodules, nasal septal perforation, and enlargement of the lips or nose. The voice also alters if the larynx is involved. Unattractive tissue damage and scarring can result from ulcerated lesions.
The general symptoms and signs of leishmaniasis can include
- Weight loss
- Pancytopenia; Low blood counts
- Hepatosplenomegaly; enlargement of the liver and spleen
- Distended abdomen
- Fever
- Skin bumps or sores that have the same presentation as acne, warts, or psoriasis.
Prevention and Treatment Options For Leishmaniasis
To treat leishmaniasis, doctors use drugs that are appropriate for the patient’s country of origin, the parasite’s species, and the type of leishmaniasis they have.
Use of Nets
Employing bed nets, protective clothing, and insect repellents can help people who live, work, or travel in affected areas lower their risk. These safety measures are especially crucial from dusk until dawn when sand flies are most active.
Drugs
There is currently no preferred drug or treatment for leishmaniasis due to the wide variety of species and manifestations as well as the paucity of extensive data. Depending on the species, syndrome type, and geographic location, medical professionals must tailor their treatments.
Amphotericin B liposomes and miltefosine
Amphotericin B liposomes and miltefosine are the only anti-leishmaniasis with FDA approval in the United States. Amphotericin B is FDA-approved for VL but frequently has side effects, including renal toxicity.
Miltefosine (Impavido) is FDA-approved for treating CL, VL, and ML brought on by Leishmania braziliensis, L. Patients typically tolerate miltefosine well. L. aegypti, and guyanensis. It is the first oral VL treatment that is highly active.
Antifungals
Azole antifungals fluconazole and ketoconazole may be effective against particular species of fungus. Infested people can administer pentavalent antimonial (SbV) compounds, which are conventional antimony-based medications, intravenously or intramuscularly.
The United States has sodium stibogluconate (Pentostam) on hand. There are high rates of VL that is resistant to medication in some places, like the Indian state of Bihar.
Bihar has experienced success with liposomal amphotericin B or even short-course amphotericin B. Pentamidine has a variety of toxicities and has been employed as a second-line treatment for VL.
Given the seriousness of the lesion, CL in a person with normal immunity may not necessitate any treatment because it will go away on its own in a few weeks. Sometimes medical professionals will only keep an eye on cases with a few slight lesions that seem to be healing.
Medication is used to treat quite severe disease cases, but the best course of action depends on where the disease may have been contracted and the Leishmania species.
Oral ketoconazole (Nizoral, Xolegel, Kuric, Extina), and Leshcutan; a topical 15% paromomycin compound are potential treatment options for case scenarios that arrive in the United States. Other treatments include local heat therapy (which needs local anesthesia) or repeated cryotherapy using liquid nitrogen over weeks.
Permethrin
Permethrin is applied to the apparel to make it insect-resistant, and the apparel is re-treated after about five washings. Use topical insecticides like Adantix or an insecticide-containing collar like Scalibor, which typically contains deltamethrin, on domestic dogs that must travel to locations where contagious. Dogs should also be kept inside during the evenings. Throughout Europe, there is a canine anti-leishmanial vaccine called Cani Leish.
It’s crucial to speak with the CDC and a doctor who specializes in infectious diseases because mucocutaneous leishmaniasis is less common and there isn’t a clear treatment standard. In a broader sense, treating infected animals and people as well as using insecticide sparingly may be able to decrease the incidence of infection in endemic regions.
Read Also: Kwashiorkor: Definition, Symptoms, Causes & Treatment
Conclusion
Leishmaniasis is an infection that affects many different body parts and is caused by a variety of Leishmania species. According to the type of present, leishmaniasis symptoms and signs typically vary.
To treat leishmaniasis, doctors use drugs that are appropriate for the patient’s country of origin, the parasite’s species, and the type they have.